Watch an exclusive video of 2018-2019 ASCO president Dr. Monica M. Bertagnolli delivering her Presidential Address at the Opening Session of 2019 ASCO Annual Meeting on Saturday, June 1, 2019, and read the full text of her remarks. Learn more about Dr. Bertagnolli's experience visiting communities around the United States during her presidential term.
Welcome, everyone. We are so glad that you are all here today. Those of you attending your first ASCO Annual Meeting: Welcome to this amazing organization. What I’d like to do is to show you some of what ASCO offers, and challenge you all to join in to make a powerful future a reality.
We have a tremendous responsibility, not just to do what we are most capable of, today, but to make sure that we use every single opportunity to make progress—to do better in the future until suffering from cancer is no longer part of our world.
Caring for every patient, learning from every patient is our theme this year. It says a lot about who you all are and what you can do. You—in this room, and in this organization—are accomplishing great things, with incredible skill, dedication, and resourcefulness. Take a look around you. We have in this audience today our mentors, our heroes, our friends, our colleagues, and our students.
I am in awe of the knowledge and experience in this room right now. Think about how hard you have worked to get where you are today. Think about what you have done with—and for—so many people who needed your expertise, over just the past year.
Now, ask yourself a question. What if the next time you and your patient had a challenging decision to make, you could draw upon the knowledge and experience of everyone in this room today?
Hold that thought. We’ll be back to it later. But first, I want to share some of what I have learned from ASCO members during my year as your president.
Caring for every patient, learning from every patient: What does that mean?
It means that every person with cancer will have access to high-quality care, and also will have the opportunity to participate in clinical research. The important word here is every.
We know that this is not the case today—that disparities in access to care and clinical research are widespread, and the tricky thing about disparities is that their causes are complex. Their roots go deeply into the communities that we serve. We simply cannot address disparities in care without understanding more about them. To illustrate this, I traveled with ASCO staff members and colleagues to some regions of the U.S. that are dealing with particularly difficult issues.
I had the great privilege of seeing, firsthand, what ASCO members bring to these communities.
First, we went to Appalachian Ohio, where cancer incidence is higher and treatment success is lower when compared to the nation overall. But some physicians, health care workers, and advocates are working hard to change that. Dr. Electra Paskett of The Ohio State University introduced Dr. Colin Weekes and me to community-based programs that promote access to cancer screening and prevention across the economically deprived counties of Appalachian Ohio. These programs are crucial in promoting access to cancer screening and prevention.
We also visited ASCO members Dr. Srini Vasan, a radiation oncologist and Dr. Utpal Bhanja, a medical oncologist. They care for patients at the Strecker Cancer Center of Marietta Memorial Hospital. Drs. Vasan and Bhanja also ensure access to clinical trials by serving as an NCI-funded NCORP site.
For the members of the Oglala Sioux Nation in Kyle, South Dakota, anything beyond basic primary care, such as chemotherapy, radiation, or cancer surgery, is at least 90 miles away! Poverty is widespread, and the life expectancy for residents of the Pine Ridge Indian reservation is the lowest in the nation—just 49 years for men, and 52 years for women. At the Kyle Youth Center, Cece and John Haas hosted us during a meeting of the Pine Ridge Cancer Support Group. There, we learned that the difference between receiving needed cancer care or going without can come down to the affordability of a tank of gas.
In Rapid City, South Dakota, the closest location for cancer treatment, ASCO member and radiation oncologist Dr. Daniel Petereit treats many patients from Pine Ridge. For the past 16 years, he has directed the Walking Forward Program, bringing cancer control and prevention clinical trials to Pine Ridge.
Laredo, Texas, is a southern U.S. border town of about 285,000 people. It has five bridges across the Rio Grande linking it to the Mexican states of Tamaulipas and Nuevo Leon. Patients diagnosed with breast cancer at the federally funded Gateway Community Health Center in Laredo not only receive the care that they need, but can also participate in NCTN clinical trials. That’s because of the efforts of ASCO members Dr. Gary Unzeitig and Eduardo Miranda. Still, for the more than 50% of Gateway clients with no health insurance, securing the necessary medications and services often requires, in Gary’s words, a “hand-to-mouth” approach.
Queens, New York, is the fifth largest city in the U.S. There are 108 different languages spoken in Queens, and a majority of its residents belong to underrepresented minority populations. Many citizens of Queens face exceptional social challenges, such as homelessness and food insecurity. For them, a cancer diagnosis is sometimes not even their biggest problem.
Dr. Peggy Kemeny, professor of surgery at Mt. Sinai’s Icahn School of Medicine, has made it her mission to care for, and learn from, these special patients. Since her arrival in 2001, her leadership has created a place where cancer care is possible because the patient’s social needs are also addressed. Her lifesaving work has also led to clinical trials participation for almost 1,000 patients at Queens Hospital Cancer Center.
We also made visits to Puerto Rico, where the oncology community faced the devastation of Hurricane Maria with courage and resourcefulness, and Sidney, Montana—a prairie town that has established a high-quality cancer treatment center to serve a rural community spread across 200 miles in every direction.
While limits on how much I could travel in a year kept my community visits within the United States, one-third of ASCO members are from outside of the U.S. Thanks to international representatives on the ASCO Board of Directors, Dr. Jaap Verweij and Dr. Tony Mok, you can find more inspiring stories from Germany and Hong Kong on Cancer.Net.
So now we turn to you, in this room today. Please take out your smartphone, open up the Interact app and use it to tell everyone here something about yourself. Please type in one to two words that describe you. What country are you from? Do you practice in an academic medical center? A community practice? What is your subspecialty? Even more important, are you yourself a cancer survivor? A caregiver for a patient with cancer? Whatever you want to share that describes you, type it in. Multiple responses are fine.

I hope that the last few minutes have also allowed you to reflect a bit, and appreciate what you personally contribute to the noble work that we do.
The exciting part of being in cancer treatment today is not just the scientific breakthroughs we celebrate at this Annual Meeting—and they are exciting—but the dynamic of what can happen when two other major forces come together to propel health care forward: the power of the smart, skilled, and dedicated people in our organization, and the amazing potential of our society’s new era of interconnectivity.
Think about it.
Caring for every patient, learning from every patient.
What a powerful vehicle for progress we would have if every person challenged by a cancer diagnosis had access to the care that they need. Think about how powerful it would be if every person’s experience could contribute to making a better future.
We know that we fall short of this now. ASCO committees, populated by volunteers from among all of you, are working hard to understand why this is the case. They’re assessing needs and barriers, and developing strategies to achieve our vision; that vision is a world where cancer is prevented or cured, and every survivor is healthy.
Looking at the names of the ASCO volunteer groups tells you something about the broad scope of this work: it is as broad as our society. It intersects with where we live and work, what laws govern us, what principles underlie our ethics, where our parents came from. The work, in short, dives deep into our communities. You will see progress made by these ASCO volunteer groups everywhere you turn during this Annual Meeting.
You will, of course, also see that we have a long way to go to know that we truly are doing all that we are capable of. Our world is changing so quickly. The most amazing thing is that you have the internet in your pocket. So do our patients, our patient’s family members, almost everyone in our American communities. This tool spans international borders, reaching even places were many other resources are absent, in rural America, in Sub-Saharan Africa, even in Puerto Rico during the devastation created by Hurricane Maria.
Think about how much our world has changed in just the past decade. In 2009, the smartphone was only 2 years old, and 15% of Americans had one. Today, this figure is more than 80%.
In rural America, we have a health care access problem. The availability of subspecialists—like us—is much less than in urban centers. But we do have communication tools. The percentage of rural Americans with smartphones is essentially equal to that of urban centers.
In Africa, UNESCO finds that 7% of households are internet connected. One out of 14 means that there is a long way to go, but it is a highly significant start.
How about exchange of information throughout the health care environment? In 2009, 6% of physicians were using a fully functional electronic health record. Today, this figure is greater than 90%. In 2009, our patients did not have access to their electronic data. Today, all fully functional EHRs allow patients to participate in their health care by having direct access to their record.
What does this mean to our goal of caring for every patient and learning from every patient?
We have the tools to exchange information, but are we really connected in ways that help us achieve this goal? How can we use new technology to help us be better doctors?
Let’s get back to all of you. Remember that question I asked you a few minutes ago? I want you to go back to your smartphone app and help us all think about how we could all work together.
Think about the last time you were faced with a patient whose treatment planning was very challenging. How did you decide what to recommend? Did you review the current literature? Consult a colleague? Present the case to a tumor board? Go to an online resource? You undoubtedly took the best knowledge that you could find and made your own best judgment, based upon your past experience and clinical skills.
What if you could also draw upon the knowledge and experience of everyone in this room today? Imagine what would happen if we could bring the wisdom of the crowd—this crowd—into the consult room with your patient?
Let’s consider one example, a situation that is unfortunately faced by far too many people: a diagnosis of advanced non-small cell lung cancer. New data concerning how to treat this disease is rapidly accumulating, but it can still be very difficult to know what to recommend for an individual patient. I am going to ask you to use the app to tell us all what you would recommend for a 75-year-old gentleman with the following clinical situation:
- He has an advanced adenocarcinoma of the lung with no genomic changes predicting for a response to an approved targeted therapy.
- He has received first-line induction chemotherapy with a platinum-based doublet, and he fortunately had a great response.
- He tolerated his chemotherapy pretty well, but he tells you that he recently stopped playing golf—which he loves—because he now gets too tired.
- So, the drugs that you have been giving are working—but he's reaching a limit.
What now? This lovely gentleman, of course, wants to live as long and as well as he can. He wants to enjoy the time that he has left.
Let’s see what the wisdom of this crowd says today. Using your app, tell us what you recommend:
- Pemetrexed maintenance therapy
- Anti-PD-1/PD-L1-directed maintenance therapy
- Anti-PD-1/PD-L1-directed therapy at next progression
- Other, including supportive care
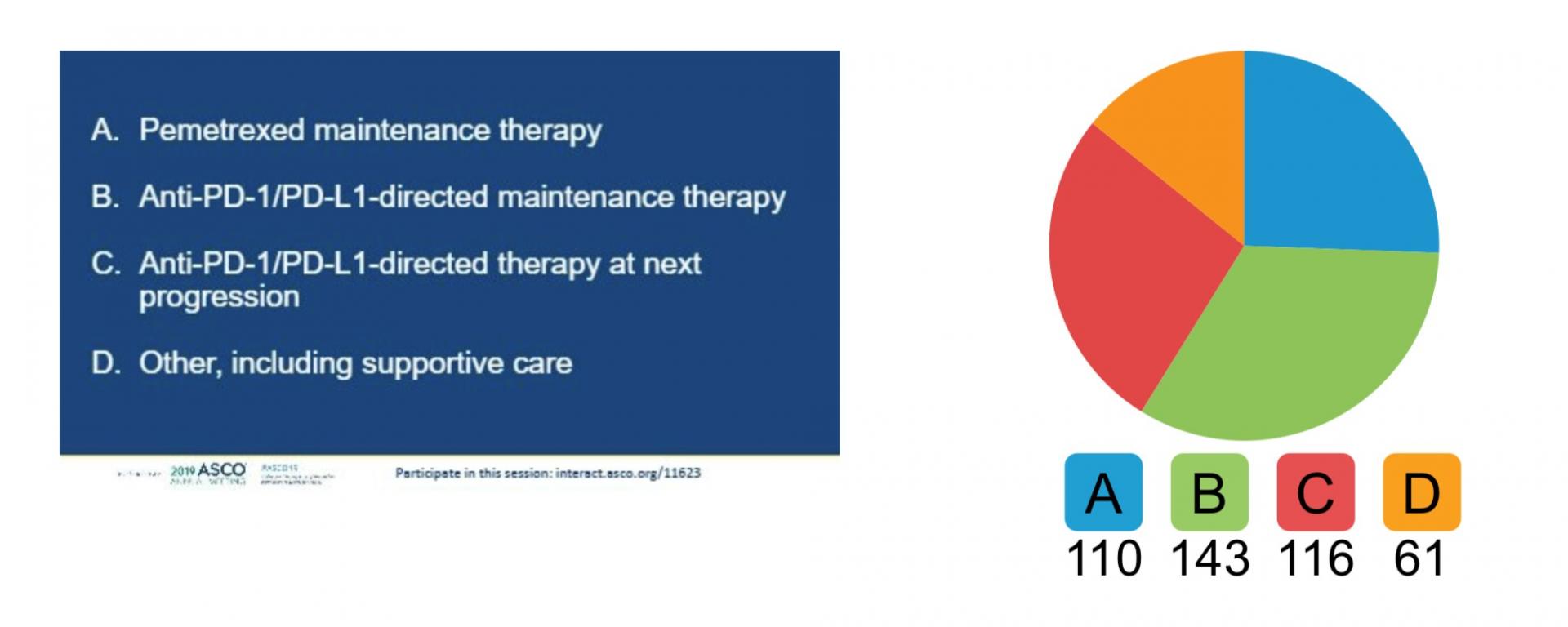
Above: Live results of the audience-response poll.
Using data available today, we can estimate the outcomes of these different approaches. Real-world datasets from ASCO’s CancerLinQ® captures information on older adults—those not typically included in randomized clinical trials.
This shows that, for a 75-year-old gentleman with a decline in strength, continuing to treat with pemetrexed in a maintenance approach is feasible, and can be tolerated for a duration that clinical trials tell us produces a 3-month increase in overall survival, compared to supportive care. Additional studies also indicate that switching to anti-PD1-directed therapy can increase survival duration, sometimes dramatically, but only in a subset of patients—about 20% of patients like this—and this treatment is very expensive.
So, you see, even with the best information available today you and your patient will still need to make a difficult decision together. All of us can see that our decisions can be better if we have the best available information at our fingertips every time we meet with a patient.
But we still need to do much more.
The wisdom of the crowd tells us that judgments—those tricky decisions that can’t be made simply by following algorithms or pathways—can be better when made by large groups than when made by individual experts. But—and this is a very key point—this is only true when the crowd is deciding based upon high-quality data, which means that we need to capture data that accurately reports the status of your patients and the results of treatment decisions that you make together.
I want each of you to think back on what happened to your patients over the past year or two. How many treatments were successful? How many were disappointments? How many times did hindsight cause you to wish you had taken a different approach? Most importantly, do you think you are better at making decisions now than you were when you first started?
Of course you do. But now think, where do we in this room go to learn from all of your results?
How many times has an altruistic patient told you: “I hope that something from my journey can be used to help someone else?” We are failing an important responsibility by not having a way to make this happen for every patient who makes this request.
Remember 10 years ago—2009? GPS capability had been around for decades, but that was the year Google Maps was first piloted in the U.S. Most of us still used printed maps to find our way around. Some of us downloaded directions from the internet before a trip, but it was still so primitive compared to today.
Now we have a smartphone or a unit in our car right in front of us that gives us the path to our destination in real time. It also allows us to make better driving decisions by showing us traffic patterns or recommending helpful detours.
In the future—hopefully the not too distant future—we will look back at today and marvel at how clumsy and primitive our electronic health records were. Just like GPS before 2009, we have a situation where the technology is available, but we can’t easily interact with it in a way that helps us get to where we need to go. I don’t pretend that practicing medicine is as simple as driving a car—far from it—but this example shows us what we need to do.
We must structure information collection, exchange, and analysis so that the EHR becomes the tool that we use to guide our clinical decisions and to learn from our results. I am sure you all know that there are significant challenges to overcome to make this future a reality. Some fundamental elements of our health care environment need to change, and this is never easy.
So, with the last few minutes, I want to describe what ASCO is doing to bring this change about.
First, we all need to be connected. As I mentioned, 90% of U.S. physicians are now using a fully functional EHR—but so few are connected so that data can be shared. This is essential. Each of our EHRs must be linked so that we can collect, aggregate, and analyze data from the clinical environment. We need to remember that the clinical data belong to the patient, not to us, and that we must honor our patient’s requests to use their data to make the world better for those facing cancer.
We also need to make a dedicated effort to ensure that these data include underrepresented minorities, patients with rare conditions, and patients who live in rural settings. We must make sure that patients and clinicians in Laredo, Puerto Rico, Appalachia, Queens, and Pine Ridge are not left out.
To achieve this, ASCO is building CancerLinQ.
You have seen a glimpse of what CancerLinQ can do today, but this is just the very beginning. CancerLinQ is still an infant, taking its first steps, and there is a lot of growth and investment to come to achieve its potential. It has been built so far through generous support from those of you who donate to the Conquer Cancer, the ASCO Foundation, and with many hours from ASCO volunteers.
Think of what CancerLinQ will do when it fully connects all of us and learns from all of our patients’ experiences. Artificial intelligence—machine learning—is a tool that can reveal important new insights from large datasets. The potential of this technology is tremendous, but again, without high-quality data that accurately represents the clinical environment, without investment of your knowledge and experience, machine learning is far less useful and might even produce results that are harmfully misleading.
To make sure that our patient’s results are accurately recorded, we need a shared language for our medical data. How many times have you struggled through a medical record from a different institution, trying to piece together the information needed to treat a patient?
We need to build a common, structured language for every EHR, making the data computable, for analysis at scale so that we routinely and accurately capture the information we need to care for and learn from our patients. ASCO has convened an initiative to develop and disseminate this language, known as mCODE, which stands for minimal common oncology data elements.
The process of building this language is iterative and highly collaborative. Other organizations currently involved in mCODE development include MITRE Corporation, the FDA, the National Cancer Institute, and the Alliance Foundation, and the list of mCODE users and developers continues to grow. By sharing your decisions and results using the common mCODE language, you will make sure that translation errors don’t limit the quality of the information that you and your patient contribute to the learning environment.
Finally, it is important that our connectivity flows both ways. We must invite our patients to participate. The doctor-patient relationship is a partnership, built upon trust that is established through honest communication. We will all be much better doctors when patients are able to easily access their information, to know how their information is being used, and to give consent for participation in research. ASCO and CancerLinQ are defining a prototype for a patient engagement portal, funded by Conquer Cancer, to achieve this goal.
And now, I ask that you take out your smartphone one more time. I have one final request of you all.
I want you to do something to demonstrate better than I ever can just why it is so important for us to achieve this vision of uniting through information technology to care for every patient and learn from every patient.
Take out your phone, and use one or two words to tell us: What do you know best? What special area of knowledge do you bring to the world of oncology? What can we all count on you to contribute to the wisdom of the crowd?

It has been the greatest honor of my career to serve as the president of our organization—a community that is dedicated to bringing about a world where cancer is prevented or cured, and every survivor is healthy.
In closing today, I want to thank and acknowledge you all, and to celebrate the contributions of the 45,000 ASCO members across the globe who bring your knowledge, your judgment, and, most of all, your humanity to this task.



Recent posts