Originally published on prost8blog; republished with permission.
The July 3 issue of JAMA Network contained a disturbing article regarding the risk of developing Alzheimer’s disease or dementia following use of androgen deprivation therapy (ADT). Using the SEER-Medicare database, the authors identified a cohort of men age 66 or older who were diagnosed with localized or advanced prostate cancer between 1996 and 2003. The data on what happened to them in the next 10 years were then analyzed according to whether they received ADT or not in the 2 years following their diagnosis. These were older men (74 to 76) who mostly lived in metropolitan areas; three-quarters of the participants were white, two-thirds were married, with just over one-third coming from low socioeconomic backgrounds. There were 62,330 men who received ADT and 91,759 who did not in the final groups analyzed.
With a mean follow-up of 8.3 years, the risk of developing Alzheimer’s disease among the control group was 9.4% but increased to 13.1% if the men received ADT (p < 0.01). Similarly, a diagnosis of dementia increased from 15.8% to 21.6% with ADT exposure, and there was evidence that the longer the men were on ADT, the worse the risk. These data are disturbing to me on two levels. First, I was unaware that 75-year-old men have such a high risk for developing Alzheimer’s disease or dementia in their next decade; and second, as a frequent prescriber of ADT for men with prostate cancer in general, and particularly for those receiving curative-intent radiotherapy for high-risk disease, it adds to the challenge of how long to recommend such therapy (if at all).
The risk curve for Alzheimer’s is shown in this figure:

The benefit of adding ADT to curative-intent radiotherapy has been demonstrated in a large number of studies dating back to the 1990s. For example, one of the most cited studies compared the survival and prostate cancer-specific survival of adding 3 or 6 months of hormone therapy to radiotherapy in patients with advanced local disease. The advantage of 6 months (compared to none or 3 months) of ADT is shown in this figure, and is about 10%, somewhat better than the increased risk of developing Alzheimer’s that is probably created.
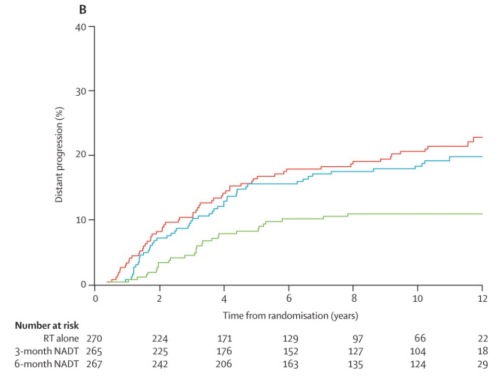
The details of these kinds of comparisons are quite complicated: for example, trying to separate out various categories of “high risk” or “higher risk” prostate cancer, etc., as reflected in this editorial by Dr. D’Amico. Numerous other studies continue to support the use of ADT to improve outcomes of radiotherapy, the challenge being how long to continue it and weighing toxicities (cardiac, quality of life, dementia risk, etc.) versus the advantage in terms of prostate cancer control. Dr. D’Amico looks forward to better information in his final statement, “During the next few years, data that will shed light on whether more than 6 months of AST is needed to prolong survival in men treated with RT for localized high risk or locally advanced prostate cancer will be provided by the completed EORTC randomized study 22961.”
Stay tuned, and if you are a patient who has been told to take ADT to improve the outcome of radiation to your high-risk localized prostate cancer, discuss the details with your physicians! How old you are, what is in your family history, and your own thoughts regarding risks of prostate cancer recurrence/death or dementia are important issues.


Recent posts