Jun 30, 2015
Introduction
By Jeffrey A. Meyerhardt, MD, MPH
Dana-Farber Cancer Institute
Each year, over 1.6 million Americans and 14 million people worldwide are diagnosed with cancer. Further, cancer causes the deaths of 600,000 people annually in the United States and over eight million people globally. It is estimated that only 5% to 10% of these cases can be attributed to inherited genetic abnormalities, while 90% to 95% have their roots in the environment and lifestyle.
Many of these exposures are modifiable in that individuals can alter their diet and level of exercise; limit sun exposure; and avoid tobacco use and exposure to secondhand smoke, to name a few of the top modifiable factors. It can be argued that data on the preventative effects of certain exposures, for example fruit and vegetable intake, are mixed and lead to confusion about best recommendations for patients. However, the data on the benefits of exercise are fairly consistent for multiple cancer types, as well as for cardiovascular disease, diabetes, and other comorbidities.
Further, the potential mechanisms by which exercise prevents cancer may also be important for patients with established cancer. Indeed, there are emerging data from prospective observational studies that breast and colorectal cancer survivors, and likely survivors of other cancer types, have a reduced risk of recurrence and improved survival if they are physically active.
In this issue of ASCO Connection, Dr. Lee W. Jones dives into the biology of exercise, focusing on the various proposed mechanisms by which exercise can lead to tumor development and progression. Understanding this biology will further advance the fields of both prevention and survivorship for multiple cancer types.
Dr. Meyerhardt is the Clinical Director and Senior Physician at the Gastrointestinal Cancer Center, Dana-Farber Cancer Institute, and an Associate Professor of Medicine at Harvard Medical School. He has been an ASCO member since 2002 and is an Associate Editor for the Cancer.Net Editorial Board. Dr. Meyerhardt has served on multiple ASCO committees and is currently the Co-Chair of the Gastrointestinal Guideline Advisory Group.
Exercise in Cancer Prevention and Prognosis: Alterations of the Host-Tumor Interaction
By Lee W. Jones, PhD
Memorial Sloan Kettering Cancer Center
The putative benefits of regular exercise on both the primary and secondary prevention of major chronic conditions such as heart disease, stroke, and type II diabetes are established. As a result, in the prevention and treatment of the most common chronic diseases, recommendations to increase regular exercise are viewed as being of equal importance to smoking cessation, maintaining a body mass index (BMI) of less than 25 kg/m2, and consuming a balanced diet.1
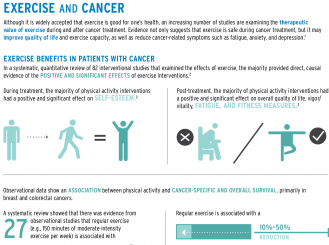
In contrast, the notion that exercise may prevent the incidence of certain forms of cancer has not gained the same level of clinical acceptance. The underlying reasons for this difference are not known; however, there is now convincing observational evidence that participation in exercise is associated with a 30% to 50% reduction in the primary incidence of colon and breast cancers, as well as a 10% to 30% reduction in the risk of other common cancers, such as prostate and lung cancers.2 Similarly, researchers have only recently begun investigating whether modifiable host factors influencing energy balance, such as body size, diet, and physical activity and exercise, are associated with cancer outcomes post-diagnosis.3,4 Regarding the latter, several observational studies suggest that, in general, regular physical activity is associated with a 10% to 50% reduction in the risk of recurrence, as well as cancer-specific death, even after adjustment for confounding factors, such as BMI, age, and adjuvant therapy.5,6 The majority of work has been performed in early-stage breast cancer, but initial evidence also exists in early colorectal, prostate, and ovarian cancers.5,6
Together, these data have led to a growing consensus that exercise exposure after a cancer diagnosis may alter cancer outcomes, fueling calls to action for confirmatory phase III randomized trials.4,7 Indeed, at least one such trial is ongoing. The Colon Health and Life-Long Exercise Change (CHALLENGE) trial is a phase III trial investigating the effects of regular exercise on recurrence and cancer-specific mortality in patients with postoperative colorectal cancer.8 The results of this trial are eagerly anticipated and will provide new insights into the efficacy of exercise to alter the clinical course of progression. In conjunction with such efforts—similar to the development of new anticancer agents—a thorough understanding of the biologic properties, optimal dose, and predictive biomarkers to inform patient selection will optimize the therapeutic benefit of exercise as adjuvant therapy. A brief overview of emerging data in this area is summarized here.
The biology of exercise
Exercise is planned activity requiring the sustained activation of skeletal muscle with the objective of improving health or fitness. Adenosine triphosphate is required to maintain muscular work in response to exercise, resulting in the mobilization and breakdown of intramuscular and extramuscular substrates (e.g., carbohydrates and fat) in combination with the delivery of oxygen (from the atmosphere, via the organ components of oxygen transport) to match the muscle metabolic requirements during prolonged exercise.9 The complex, coordinated multiorgan response that controls and regulates the physiologic response to exercise has been summarized by several excellent reviews.10-12 In brief, repeated muscle contraction in response to chronic, repeated exercise stimuli leads to the activation of a multitude of gene-expression pathways promoting several local adaptive physiologic responses. Intriguingly, these local physiologic adaptations may represent primary events that, in turn, initiate a complex cascade of subsequent local and systemic events that profoundly modulate whole-body (host) physiology and host milieu.
Exercise modulation of the systemic (host) milieu: Is muscle a key link?
The prevailing model is that exercise may alter the events underlying cancer initiation and/or progression via the modulation of circulating growth factors and other cell phenotypes representing metabolic, sex-steroid, immune-inflammatory, and oxidative pathways that comprise the systemic host milieu.13 In this realm, most research to date has focused on the role of exercise in modulating circulating metabolic factors. Skeletal muscle is the major tissue responsible for both insulin-stimulated glucose uptake and fat oxidation and accounts for approximately 80% of glucose disposal under insulin-stimulated conditions; exercise can increase glucose uptake 20- to 100-fold in the muscle via insulin-independent mechanisms.14 Consequently, increased exercise-induced glucose disposal is critical to maintaining normal whole-body metabolic homeostasis, but it also improves metabolic control among individuals with abnormal glucose control.15 In cancer, elevated circulating levels of glucose, insulin, and insulin-like growth factors are associated with a higher primary risk of certain forms of cancer, as well as poorer prognosis after a cancer diagnosis.16 As such, the well-established ability of chronic exercise, particularly endurance exercise training, to favorably modulate the metabolic profile in the peripheral circulation is likely an important mechanism underlying the exercise-cancer relationship. Unfortunately, this hypothesis has not been directly tested and the limited number of clinical studies examining the effects of exercise on changes in circulating metabolic factors in patients with or at risk of cancer are mixed.5
Surprisingly little is known about the effects and molecular mechanisms of exercise-induced regulation of the other cancer-implicated host pathways.17 Such effects are likely governed by a highly integrative, complex cascade of signaling events involving numerous positive and negative reciprocal feedback loops between numerous organ systems, orchestrated via instructive signals delivered in the host bloodstream. Primary events instigated in the skeletal muscle action may again play a critical mediating role in this process. For example, recent discoveries indicate that in response to chronic exercise, skeletal muscle operates as an endocrine organ, secreting various factors both locally and into the host circulation. In this way, skeletal muscle exerts endocrine and autocrine effects within other organs, including the brain, liver, bone marrow, pancreas, and adipose tissue (i.e., muscle-organ crosstalk).18 Such effects not only are likely to influence the release of factors from these distant organs, thus altering the nature and concentration of circulating factors in the systemic milieu, but may also directly modify the tissue microenvironment (niche) of these organs. This latter effect could play a role in recurrence because distant organs that may engage in crosstalk with muscles could harbor disseminated cancer cells; exercise-induced changes in the systemic milieu could, in turn, alter ligand availability in distant organ (metastatic) niches to potentially affect escape from dormancy and/ or progression of overt metastases.19 Although potentially exciting, such a concept remains pure speculation at present and will require transdisciplinary research efforts to address.
Are tumor subtypes important?
Research investigating the mechanisms by which exercise may prevent primary or secondary cancer incidence has, to date, focused exclusively on modulation of circulating factors in the peripheral (host) circulation. As an extension, it seems biologically plausible that tumor cell response, and/or response of cells in the tumor microenvironment, to exercise-induced changes in host factors will also vary dramatically based on the tumor molecular profile.
A small number of initial studies have investigated whether tumor molecular features modulate the exercise response. For example, Holmes et al. found that regular exercise (i.e., approximately 150 minutes of moderateintensity endurance exercise per week) was associated with a relative risk reduction in breast cancer death of only 9% in women with estrogen receptor–negative tumors, relative to a 50% reduction in women with estrogen receptor–positive tumors.20 This finding was corroborated by Irwin et al.21 In a detailed analysis of tumor samples obtained at the time of surgical resection, Morikawa et al. found that patients who reported a level of exercise greater than or equal to 18 metabolic equivalent task–hours per week, and whose tumors did not express CTNNB1 (ß-catenin)—a key mediator of the Wnt signaling pathway that plays an important role in colorectal carcinogenesis—had an adjusted hazard ratio (HR) for colorectal cancer– specific survival of 0.33 (95% CI [0.13, 0.81]) compared with patients reporting less than 18 metabolic equivalent task–hours per week.1,22 Conversely, there was no significant relationship between exercise and prognosis in patients with tumors that were positive for nuclear CTNNB1 (adjusted HR 1.07, 95% CI [0.50, 2.30]). These initial findings indicate that, perhaps unsurprisingly, tumor response to exercise will likely be highly contingent on the tumor molecular landscape, similar to therapeutic response to pharmacologic anticancer agents.
Over the past decade, the safety and benefits of exercise as an effective adjunct therapy to offset the acute and late-occurring effects of adjuvant therapy have gained increasing recognition and acceptance.23 It is now clear that a parallel line of research investigating the efficacy of exercise as primary treatment for cancer is also gaining considerable momentum. In this context, exercise may represent a promising strategy with a largely unique ability to simultaneously modulate multiple host-related pathways, and potentially, therefore, the host-tumor interaction. Future efforts adopting translational approaches in an attempt to disentangle the complex multifaceted interactions between exercise-induced physiologic responses, the host milieu, and cancer phenotypes pose a substantial challenge, but could produce significant dividends in the long run.
Dr. Jones is a researcher at Memorial Sloan Kettering Cancer Center. He has been an ASCO member since 2005 and is a member of the Journal of Clinical Oncology Editorial Board, the Cancer Survivorship Committee, and the Cardiac Dysfunction Expert Panel.
References
- Eyre H, Kahn R, Robertson RM, et al. CA Cancer J Clin. 2004;54:190-207.
- Friedenreich CM, Orenstein MR. J Nutr. 2002;132:3456S-64S.
- Goodwin PJ, Meyerhardt JA, Hursting SD. J Clin Oncol. 2010;28:4019-21.
- Ligibel JA, Alfano CM, Courneya KS, et al. J Clin Oncol. 2014;32:3568-74.
- Betof AS, Dewhirst MW, Jones LW. Brain Behav Immun. 2013;30: Suppl S75-S87.
- Ballard-Barbash R, Friedenreich CM, Courneya KS, et al. J Natl Cancer Inst. 2012;104:815-40.
- Ballard-Barbash R, Hunsberger S, Alciati MH, et al. J Natl Cancer Inst. 2009;101: 630-43.
- Courneya KS, Booth CM, Gill S, et al. Curr Oncol. 2008;15:279-85.
- Jones LW, Eves ND, Haykowsky M, et al. Lancet Oncol. 2009;10:598-605.
- Hawley JA, Hargreaves M, Joyner MJ, et al. Cell. 2014;159:738-49.
- Jones NL, Killian KJ. N Engl J Med. 2000; 343:632-41.
- Coffey VG, Hawley JA. Sports Med. 2007; 37:737-63.
- McTiernan A. Nat Rev Cancer. 2008;8: 205-11.
- Goodyear LJ, Kahn BB. Annu Rev Med. 1998;49:235-61.
- Stanford KI, Goodyear LJ. Adv Physiol Educ. 2014;38:308-14.
- Pollak M. Nat Rev Cancer. 2012;12:159-69.
- Handschin C, Spiegelman BM. Nature. 2008;454:463-9.
- Pedersen BK, Febbraio MA. Nat Rev Endocrinol. 2012;8:457-65.
- Jones LW, Antonelli J, Masko EM, et al. J Appl Physiol (1985). 2012;113:263-72.
- Holmes MD, Chen WY, Feskanich D, et al. JAMA. 2005;293:2479-86.
- Irwin ML, Smith AW, McTiernan A, et al. J Clin Oncol. 2008;26:3958-64.
- Morikawa T, Kuchiba A, Yamauchi M, et al. JAMA. 2011;305:1685-94.
- Jones LW, Alfano CM. Acta Oncol. 2013; 52:195-215.