May 30, 2015
Watch an exclusive video of Dr. Peter Yu delivering his Presidential Address at the 51st Annual Meeting of the American Society of Clinical Oncology. Scroll down below the video for the complete transcript of his address.
The shift to a value-based health care system, the advent of precision medicine, and the transition to digital health are forces driving unprecedented change in oncology. These are changes that will transform medicine within the professional lives of most everyone in this hall today. Ladies and gentlemen: how we respond to these changes will determine not only the future of our profession, but the health, comfort, and care of millions of people around the globe.
As my ancestors would say, “We live in interesting times,” but accepting the challenge of great odds with the determination to succeed is the defining virtue of an oncologist. Recalling how others before us have dealt with change can offer powerful insights. So, this morning, I want to begin with the story of a highly educated professional who lived through a period of profound transformation and upheaval. He was not an oncologist. He was not a physician. In fact, he was not even alive in this millennium.
He was Johannes Trithemius, the Abbot of Sponheim, a religious house located in Germany. In the year 1482, Trithemius was a student at the University of Heidelberg. By the age of 21, he was elected Abbot of his monastery and set out to make his religious house a seat of learning and knowledge throughout Europe.
Europe in the 15th century was a society focused almost entirely on the preservation of existing knowledge rather than the creation of new learning. Monks in abbeys hand-copied books in specialized workplaces called scriptoriums. The Abbot was true to his ambition; the abbey’s bookshelves grew from 50 to an impressive 2,000 volumes. He obtained success as success was defined by the technology of his day.
But also just like today, the Abbot’s world was changing quickly. It was the dawn of the Renaissance. Disruptive forces of new technologies and new ideas would alter society forever. As the Abbot’s monks hand-copied their manuscripts, Columbus sailed to the New World and Leonardo, Galileo, and Tycho Brahe were making astonishing advances in science. And down the road in Mainz, Johannes Gutenberg’s new printing press was not only speeding the dissemination of knowledge, it was allowing the exchange of ideas.
And so very quickly, the normative was threatened. The Abbot saw how the invention of the printing press challenged the tradition of monks copying books in the scriptorium. Faced with the challenge of the new, the Abbot wrote a book, De Laude Scriptorum, “In Praise of the Scriptorium,” passionately defending the old way of doing things. Yet, he had his book printed so that his ideas would circulate faster. This inherent tension between clinging to the old even as we embrace the new is a part of human nature and a valuable lesson for us today.
Buenos días! Good morning! Da Jia Hao!
It is my great pleasure as President of the American Society of Clinical Oncology to extend the warmest of greetings to all of our members and distinguished guests. I thank Dr. Lichter for that very kind introduction, and I join my colleague Charles Penley, Chair of the Conquer Cancer Foundation, in welcoming you to the Opening Session of ASCO’s Annual Meeting.
The theme of this year’s Meeting—transforming data into learning—is about how we use the tsunami of data generated by both precision medicine and clinical medicine to learn how to care for patients with cancer in the most compassionate, effective, and sustainable manner—learning together from every patient’s experience. ASCO is leading the move to a new data-driven era of discovery in clinical oncology.
Three critical steps are needed to transform molecular and clinical data into genuine learning:
- We must be able to assess outcomes that reflect the patient perspective.
- We have to innovate how we generate and test new hypotheses in order to accommodate the accelerated pace of precision medicine.
- We need to learn how to apply the results of clinical trials to real-world patients and real-world realities of health care delivery.
These three steps define the true value of what we do. They are the tools that transform data into knowledge and knowledge into learning. If we do not define, measure, and report the value of what we bring to patients, we will not be valued by society in turn.
Our keynote speaker, Michael Porter, has spoken to us about how patient-centered outcome measurements drive improvements in the patient experience and increase the value of health care. He reminds us that the true goal is not better or cheaper health care delivery, but better health. At this year’s Meeting, we will hear presentations about reducing short- and long-term toxicities of cancer treatment, from mitigating chemotherapy-induced hair loss to managing the health problems of long-term survivors of childhood malignancies. We need and will do more to improve palliative care and survivorship for patients with cancer. ASCO’s inaugural Palliative Care Symposium last October was highly successful, and I expect that our inaugural Survivorship Symposium in 2016 will be equally so.
For patients with cancer, the path to better health is dependent on studying the systems biology of cancer. At this session one year ago, Lee Hood shared with us his vision of the potential for precision medicine to generate enormous data sets that enable us to create new models—models that lead to more effective therapies with fewer side effects. But for now, we face a deluge of data steadily increasing in volume, velocity, and variety that underscores the importance of collecting data so that it is readily accessible, searchable, and usable.
International efforts are underway to amass large precision medicine data sets. Building on The Cancer Genome Atlas, the International Cancer Genome Consortium has been acquiring 25,000 patient biospecimens from 50 types of cancer to analyze germ-line and somatic alterations in genome, epigenome, and the transcriptome. In the United Kingdom, the 100,000 Genome Project has been launched.
We are well on the path towards building ever larger and more complex precision medicine data sets. We must also foster sharing of these data sets and the creation and adoption of technical standards to do so. But patients are more than the digitalized representation of molecular data. Alongside precision medicine is personalized medicine, the aspect of cancer care that speaks to patient preferences and behavior, the role of the environment, and clinical interventions. It is just as critical to have useful clinical data sets, such as aggregated medical records, as it is to have large molecular data sets. Both are necessary to advance discovery and improve care.
The Global Alliance for Genomics and Health is an umbrella organization of 250 members, including ASCO, which believes that human health will be advanced faster through the sharing of genomic and clinical data sets. New international technical standards will enhance interoperability of data sets and allow genotype–phenotype correlations to be modeled and tested. For example, the BRCA Challenge will accelerate our understanding of BRCA variants of uncertain significance by allowing investigators to share clinical outcomes data. CancerLinQ™ is ASCO’s revolutionary health information technology that aggregates the electronic medical records of patients with cancer to create a shared clinical dataset. CancerLinQ is one example of how the daily work of individual oncologists can be leveraged for the greater good of all.
As precision medicine begins to bear fruit, we can expect that more investigational drugs will be fast-tracked by FDA pathways such as breakthrough designations and regulatory approval based on phase I and II trials with exceptionally strong signals of efficacy. At this Meeting, we will hear about the first reports of several agents that have received breakthrough designation.
We must continue innovation that accelerates the speed at which we transform data into learning. The research infrastructure constructed over the past 50 years lacks the capacity and agility to allow us to bring new treatment advances to patients at the scale now required. To succeed, we need to re-engineer how we bring concepts to clinical trial and design clinical trials that achieve more clinically meaningful advances. A faster, more nimble approach to learning is needed.
This year ASCO issued a formal policy statement calling on the oncology community to re-address widely held assumptions about phase I studies. As shown here (Fig.1), the clinical benefit of phase I study drugs in the era of targeted treatments can be equivalent to standard treatment options, with no worse toxicity. In the past, phase I studies have been viewed as toxicity-defining studies with no therapeutic benefit. This view has been a deterrent to physician referral of patients and led to denial of insurance coverage. In this new era of targeted therapies, such a view is as anachronistic as hand-copied manuscripts.
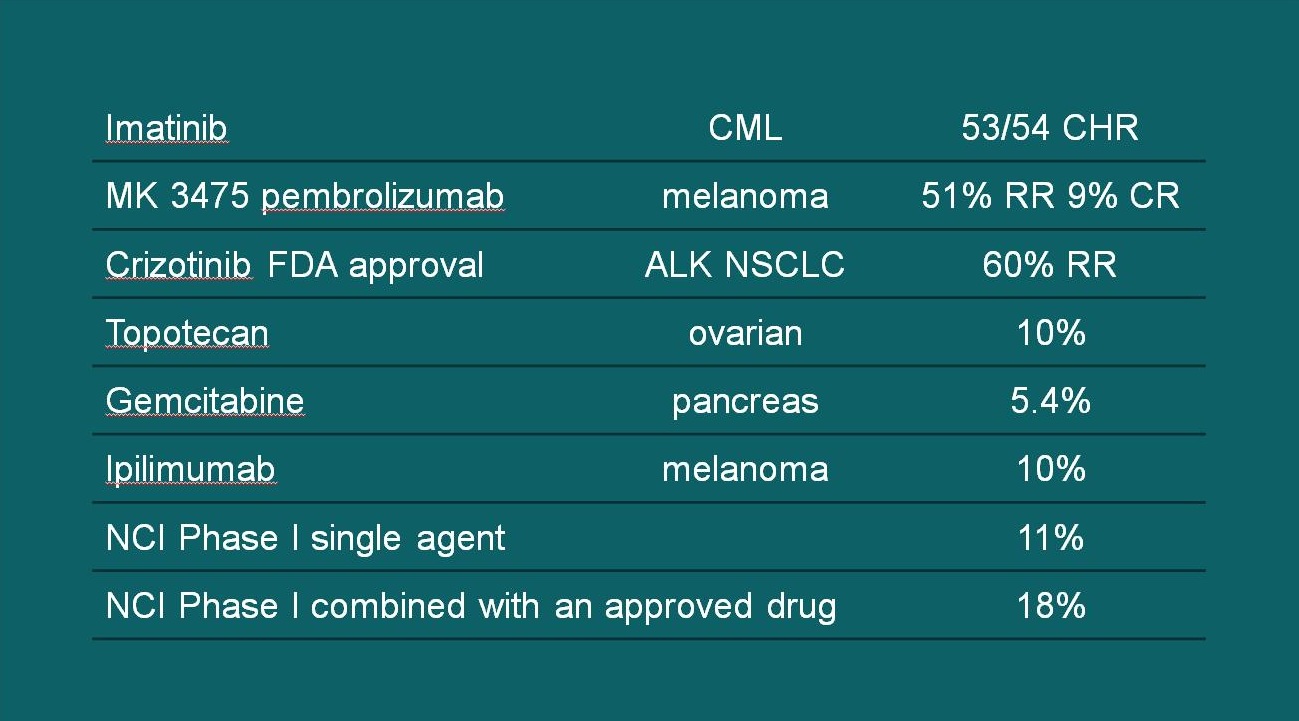
Figure 1: The clinical benefit of phase I study drugs in the era of targeted treatments can be equivalent to standard treatment options, with no worse toxicity.
ASCO has developed a model to facilitate the off-label use of targeted agents while collecting a minimal data set on safety and efficacy. Designed to study small cohorts of patients with matches of drug-to-biomarker as determined by an ASCO Molecular Tumor Board, strong early signals of efficacy will inform the design of phase II studies. Physicians and patients will benefit from a mechanism to gain access to targeted agents, and the life sciences industry will benefit by finding more promising lines of investigation. ASCO Chief Medical Officer Dr. Richard Schilsky is leading the development of this study, known as the Targeted Agent and Profiling Utilization Registry, or TAPUR study, in which pharmaceutical companies will donate their drugs. This will be ASCO’s first IRB-approved clinical trial.
Thus far this morning, we have heard of the need to measure outcomes across the full cycle of care, reflecting a patient-centered perspective. We have discussed sharing of large data sets of both precision medicine and clinical data. And third, driving innovation in knowledge generation. Finally, we come to learning how to apply knowledge in the real world of patient care, whether that is the global health of low- and medium-resourced countries or value-based medicine in the United States.
The Institute of Medicine has championed the model of a rapid learning health system that enables us to transform data into learning at a vastly accelerated pace by learning from the real-world experiences of patients. It is based on a health care system that learns from itself by continuous measurement, assessment, and improvement. Sharing of data and learning across health care providers are at the heart of Rapid Learning Health Systems. ASCO understands that a system that uses informatics to bring together clinicians across health care delivery will drive care innovation and implementation science.
Here again, I am proud to say that ASCO is out in front, leading. Since January, ASCO and SAP have combined our resources for the co-innovation of CancerLinQ, the world’s first rapid learning health system for oncology. The SAP HANA system is an in-memory data management system whose data architecture and data mining tools are the reasons why SAP is the leading enterprise data company in so many industries. HANA is the digital health platform that will underlie CancerLinQ. ASCO brings our deep knowledge of clinical oncology, and SAP brings the superior engineering prowess and project management needed to bring a new product to market. The great strength of the collaboration, however, is our mutual commitment and excitement to explore together that which yet needs to be discovered in this new frontier.
Fifteen pioneering community practices, hospital systems, and cancer centers, with great vision and dedication, have agreed to provide CancerLinQ with the entire electronic health record data of their patients; they are our vanguard practices. By year-end, digital health data from these practices will begin to flow through the CancerLinQ platform, bringing it to life. We have prepared a brief video on CancerLinQ and invite you to see the entire presentation in the Exhibit Hall.
With CancerLinQ, we have a powerful tool to study and learn from all patients, whether on clinical trials or through clinical practice. This is a transformational change that addresses a need shared by all countries and all patients with cancer. There are many ASCO programs that can be adapted to support education and quality improvement throughout the world. With international oncologists now comprising one-third of our membership, ASCO must reach out across the world to learn how we can help our members improve the state of cancer care.
In March, I traveled to South America. At the Durand Hospital in Buenos Aires, I met dedicated ASCO members who strive to provide the best patient care while working with limited resources and who self-impose an expectation that every oncologist will publish two papers each year. In Uruguay, their NCI is building an informatics infrastructure that will link electronic health records and registries, create clinical decision support tools, and establish a national bioinformatics testing and biobank facility. Traveling to Brazil, I visited a 25-physician oncology clinic that is proud of its QOPI® participation. São Paulo impresses with the extraordinary oncology care provided in private hospitals such as the Syrian-Lebanese and public hospitals such as ICSEP.
In one public hospital dedicated to the treatment of women with cancer, I found this poster displayed at the front of a crowded patient waiting area (Fig. 2). In Portuguese, it explains to patients the workflow for breast lesions, from imaging to biopsy, surgery, radiation, and medical oncology. At the bottom, the figure describes a 41% reduction in patients presenting with advanced disease and a 20% reduction in mortality, achieved through patient engagement in their own health care.

Figure 2: Poster from a public hospital in South America describing a 41% reduction in patients with breast cancer presenting with advanced disease and a 20% reduction in mortality, achieved through patient engagement in their own health care.
Everywhere, the dedication of ASCO members to their patients and their profession, their thirst for knowledge, and their dedication to applying that knowledge with the limited resources available are palpable. Over and over, each country demonstrated the desire to achieve the highest standards and a trust in ASCO to assist them in their endeavors. It is a trust that we must uphold.
This year’s Annual Meeting launches the Society’s Global Oncology Symposium. Each year, the symposium will highlight a high-impact cancer that may have unique or common characteristics from country to country; this year it is gastric cancer. Solutions or models that address health care delivery challenges, such as provision of pathology services in low- and medium-resourced countries, will be presented. With much of the world’s cancer community present at the Annual Meeting, the symposium provides the ideal international meeting venue for discussing global oncology.
Later this year, ASCO will launch publication of the online Journal of Global Oncology, which is the only journal dedicated to publishing original research related to cancer in low- and medium-resourced nations. The intent of the Journal of Global Oncology is to foster international collaboration among researchers, while providing mentorship to authors that will ensure that the highest editorial standards are achieved. We are fortunate to have Dr. David Kerr, a leader in global health from Oxford University, as the founding editor of this journal.
This is only a start. A presidential task force led by past ASCO President Gabriel Hortobagyi has been charged by the ASCO Board of Directors to study and advise on how our Society can contribute to improving oncology global health by supporting our members as they engage the oncology ecosystem of education, research, industry, and regulatory policy.
Ultimately, the need for an affordable, sustainable health care system is universal. Every nation on earth, regardless of how its physicians are trained, deployed, and reimbursed, is faced with the need to provide the best possible care within the financial constraints of their system. Here in the United States, this is being defined by value-based medicine and provider payment reform.
The move away from fee-for-service reimbursement to bundled payment models has begun. Secretary of Health & Human Services Sylvia Burwell has announced that by 2018, 50% of Medicare payments to physicians will be through alternative payment models. The Oncology Care Model from the Medicare Innovation Center brings together federal and private payers in a five-year pilot project of episodes of payment for chemotherapy services. And the recently enacted bill repealing the Sustainable Growth Rate formula sets in motion a series of payment reforms such as the Merit-Based Incentive Payment System, or MIPS, that will consolidate and expand the current array of performance programs, and set incentives and penalties that may be as high as 29% of total Medicare physician reimbursement.
These payment reform efforts seek to achieve the Triple Aim of the Institute of Healthcare Improvement, which is to improve the patient experience, improve population health, and reduce the cost of care. This will necessitate improved patient access to care, coordination of care through oncology medical homes, and discussions with patients on cost of care and end-of-life care.
Value of care cannot be assessed without measurement of the quality of care received. ASCO’s quality improvement program, QOPI, will be a key part of implementing any payment reform model. One of those models is ASCO’s Patient-Centered Oncology Payment, which bases reimbursement on flexible monthly bundles that reflect the acuity and complexity of the patient’s needs, a greatly simplified billing schedule, and a model that is not tied to the current fee schedule that drives physician encounter-based payment.
The last decade has been painful for community oncologists, who have suffered practice closures, mergers, and decreased incomes. We have witnessed disruptions to patient care in the setting that delivers the majority of cancer care in the United States. If community oncology is to survive, we must together find our way forward by designing and embracing new payment models that reward the achievement of patient-centered outcomes and value the work of the health care providers who care for patients with cancer.
A part of improving the value of care is raising our expectations of clinical trial results that are considered meaningful advances in patient care. With our Clinically Meaningful Outcomes Statement, ASCO has initiated that discussion. Four sets of experts evaluated current standards of care in the first-line therapy of advanced pancreatic cancer, triple-negative breast cancer, and non-small cell lung cancer, and the treatment of colon cancer refractory to standard care. Their goal was to determine the minimal improvement in overall survival that would constitute a clinically meaningful advance over current standard of care treatment. Working independently, they concluded that a clinically meaningful advance should demonstrate an HR [hazard ratio] of at least 0.8, which translates into an improvement in median overall survival of two-and-a-half to six months depending on clinical context.
ASCO’s Value Framework, scheduled to be published in the Journal of Clinical Oncology in late June, is designed to support physician and patient discussions of the clinical benefit, clinical toxicity, and financial cost of therapies that have been compared in randomized clinical trials. Patients need to have accurate information about expected benefit, toxicity, and cost, as well as a context for comparing new, and typically more expensive, treatments to standard alternatives. With this understanding, they are better equipped to make a choice that is consistent with their personal goals, preferences—and finances. At price points of $20,000 a month for new drugs, these discussions cannot be avoided any more, uncomfortable and unfamiliar as we may be with them. Ultimately, decisions will be made between patients and their health care providers. Collectively, these decisions will drive the level of demand for new diagnostics and therapeutics, which in turn may help influence more rational pricing of these products.
One of the greatest values that ASCO brings is in the nurturing of the next generation of oncologists. Since 1984, ASCO has helped launch almost 1,000 careers through our Young Investigator Awards to oncology fellows whose interests vary from translational bench research to research into improving the patient experience. This is the seed funding that provides tangible support for the innovation and energy that ensures our future. Fifty-eight YIAs, a record number, have been awarded this year, but even more would have been funded had we the resources to do so. At this meeting, the Conquer Cancer Foundation launches a $150 million dollar campaign and over one-third of the dollars donated will go to support groundbreaking research being done by both young investigators as well as more seasoned researchers. I urge you to contribute generously so that the Conquer Cancer Foundation can support oncologists who make a difference by thinking creatively.
Over the last five years, it has been my privilege to serve on the ASCO Board of Directors and have the opportunity to take a longer and broader perspective, to look back and see the incredible progress we have made over the course of 50 years, and to look forward to the future ahead. The task has been made easier and all the more rewarding working with our Chief Executive Officer Dr. Allen Lichter and the ASCO staff whose dedication to serve is equal to any of us here today and who help make ASCO the preeminent scientific and educational organization in the oncology community. Truly, it has been an honor for me to serve as the President of ASCO during this past year, and I would like to especially thank my Scientific Program Committee Chair, Dr. Alan Venook, and my Education Committee Chair, Dr. John Cox, who together have led the planning of this Meeting. It has been my great fortune to have had three outstanding leaders in oncology as mentors through my career and I owe a great debt to Drs. James Holland, Larry Norton, and John Mendelsohn.
I opened my remarks with the story of the Abbott of Sponheim, caught in the transition of interesting times and struggling to adapt to a changing world. For centuries prior, knowledge had been preserved through the hand-lettering of illuminated manuscripts such as this. These were handcrafted works of art. With a technology limited to hand and brush, knowledge was restricted to the few who possessed the requisite education, societal status, and wealth.
Then, in 1450, a new technology was invented, the printing press. Suddenly, there was a flood of knowledge and widely distributed printed materials enabled sharing of ideas that would remake the world. The Nuremberg Chronicle was one of the most influential of these books, the first encyclopedia of human knowledge. This page, from a 1493 edition that hangs in my office, is a daily reminder to me of that very special time in human history (Fig. 3). The half-century spanning the years 1450 to 1500 was a period in time when the expansion of knowledge and learning came together, when the world married illumination to innovation. Historians have honored this period in Western Civilization with its own name, the Incunabulum, or cradle.

Figure 3: Page from a 1493 edition of the Nuremberg Chronicle, considered the first encyclopedia of human knowledge.
Five centuries after Guttenberg, and a mere 50 years after the founding of the American Society of Clinical Oncology, the confluence of precision medicine, rapid learning, and digital health prepares us for a similar incunabulum in medicine. Illumination and innovation—the transformation of data into learning—evokes nothing less. Consider this third piece of art, which hangs in the home of oncologist Dr. Thomas Roberts, an ASCO member and Board member of our Conquer Cancer Foundation (Fig. 4). As you can see, it depicts a woman pondering her genome. We are tempted to ask, like a modern day Mona Lisa, what is she thinking? Is it the relationship between the humanistic side and the biologic determinants of our lives? Do all the answers to cancer lie in precision medicine and molecular testing? Is the art of medicine fading away?

Figure 4: Painting of a woman pondering her genome; photo courtesy of Dr. Thomas Roberts.
Ladies and gentlemen, honored guests: It is our responsibility to confront the challenges before us. But bearing witness to the past 50 years of progress and the drivers of disruptive change that can be wind in our sails, it is a responsibility that we are proud to accept. The first 50 years of clinical oncology saw a transformation in our understanding and treatment of the disease. Fifty years ago, cancer was not only incurable, it was a diagnosis that left patients to endure physical suffering compounded by social disgrace and ostracism. It was the sore that did not heal.
Today, as oncologists, we stand at the end of that beginning. In the next 50 years, we will work together to create an incunabulum—a period of knowledge and learning for the benefit of patients with cancer so that more patients, most patients, maybe all patients, will be cured. We owe it to patients past and present—and most of all to generations of patients yet to come—to do no less.
Thank you.

