Aug 29, 2012
The need is urgent as most patients seek medical attention only at an advanced stage of disease
As the majority of patients with cancer in the Middle East present with advanced disease, often the only treatment option is palliative care. However, one of the main obstacles to the provision of appropriate palliative care and pain treatment is the lack of training for caregivers. In the interview that follows, Middle East Cancer Consortium (MECC) Executive Director Michael Silbermann, PhD, DMD, provides a snapshot of how oncology professionals in the region address the relief and prevention of suffering for patients with cancer.
|
AC: What is the current state of cancer care in the Middle East?
Dr. Silbermann: Most countries in the Middle East lack government policies concerning cancer control and palliative care. The majority of patients with cancer are diagnosed with advanced-stage disease, and often, the only realistic treatment options are pain relief and palliative care.
Current registry data from the region indicate that the regional burden of cancer continues to increase largely because of an aging and growing local population coupled with an increasing adaptation of cancer-causing behaviors, particularly smoking.
In Western societies, curative procedures are often prioritized ahead of palliative care. The “cure at any cost” attitude of professionals along with commonly shared religious views on the sanctity of life often influence end-of-life decisions. By contrast, Islamic societies, which constitute the majority of the Middle Eastern population, are generally more accepting of death and its inevitability, which in turn has a different influence on treatment and/or care decisions.
 |
Lung cancer is the most frequently diagnosed cancer for males in Turkey, Pakistan, Morocco, and Palestine; prostate cancer is the most frequently diagnosed cancer for males in Cyprus, Israel, and Lebanon; and colorectal cancer is the most frequently diagnosed cancer for males in Jordan and Saudi Arabia.1 For women, breast cancer is the most frequently diagnosed cancer in the Middle East. The overall cancer mortality rate is higher for females than males, who often present with advanced stages of disease.
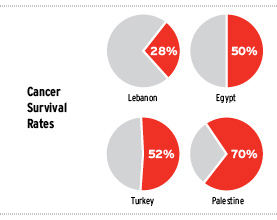
Cancer survival rates tend to be poor in certain populations mainly because of the late stage of diagnosis. For example, survival rates in Lebanon are 28%, Egypt - 50%, Turkey - 52%, and Palestine - 70%. Only a comprehensive approach that combines national policies; education of professionals and the public, including stigma reduction; early diagnosis; and access to effective treatment will guarantee success in combating cancer in the Middle East.
AC: How does palliative care fit into the overall plan for cancer control?
Dr. Silbermann: In most Middle Eastern countries, there is still a general lack of governmental policies that recognize palliative care as an essential component of health care—only Turkey and Israel have such policies. More than 50% of patients with advanced cancer experience moderate to severe pain. To date, opioids continue to be unavailable and inaccessible in sufficient quantities to most countries in the region.
Barriers to palliative care and pain treatment can be divided into three areas: 1) lack of health policies in support of palliative-care development; 2) lack of relevant training for health care professionals; and 3) poor accessibility to essential palliative-care drugs.2
MECC—jointly with the Children’s Hospitals and Clinics of Minnesota—has recently initiated training courses and workshops for health professionals across the region. The goal of these educational activities is to create a Middle Eastern nucleus of champions who will facilitate continuing educational activities throughout the region. In recent months, “MECC graduates” have initiated and organized training activities in Jordan, Palestine, Egypt, and Cyprus.
In January, the General Assembly of the United Nations adopted a revised resolution to its September 2011 Political Declaration, which emphasized the importance of palliative-care services, especially in developing countries. This fact is relevant to most Middle Eastern countries, where most patients with cancer seek medical attention only when the disease is in an advanced stage, beyond cure, but are suffering from severe pain and other disabling symptoms. Hence, countries with limited resources should consider home-based palliative-care services, which can be provided, for the most part, by a visiting nurse with a community health care worker under the supervision of a physician either in the community or in an oncology center.
Two non-governmental organizations in Cyprus, the Cyprus Anti-Cancer Society and the Cyprus Association of Cancer Patients and Friends, have succeeded in developing a national model for such an efficient palliative-care service.
AC: What is your role in the development of palliative-care services, and what changes do you envision?
Dr. Silbermann: The Middle East is characterized by multiple faiths and cultures, and it is imperative that health care providers are respectful of and responsive to the various health beliefs, practices, and cultural needs of such a diverse population.
MECC’s palliative-care project will place much emphasis on end-of-life care. It is MECC’s immediate goal to enhance education at all levels, including families, health care professionals, religious officials, policymakers, and regulators. Psycho-oncology and palliative care are concurrently evolving subspecialties around the world. In developed countries, these subspecialties are beginning to focus on the psychological, behavioral, physical, spiritual, and existential dimensions of patients with cancer, their families, and caregivers. MECC has begun to introduce these important facets in its training activities in the region. It is MECC’s hope that initiatives and efforts of international organizations such as ASCO will help ameliorate significant mental and physical health care disparities in the Middle East.
AC: Is there anything else you would like to share?
Dr. Silbermann: Pain management has been surrounded by myth, irrationality, and cultural bias in the Middle East. It is MECC’s belief that education and training are the cornerstones of improving palliative-care services.
References

