It’s been almost three years since the National Lung Screening Trial (NLST) reported a 20% reduction in lung cancer mortality. Why is it taking so long to see low-dose CT screening become a reality?
We’re getting closer. The U.S. Preventive Services Task Force (USPSTF) has rated lung cancer screening “B”, meaning it will be covered by private insurance. But recent hearings by MEDCAC, the Medicare Evidence Development & Coverage Advisory Committee, resulted in a “low confidence” vote and may influence the decision for Medicare coverage.
How can the government both sanction private insurers covering screening and yet deny it to patients 65 and older? It smacks of ageism, but it’s partly because there are some fundamental issues that need to be resolved. I think if critics and advocates are willing to work together, it’s achievable.
Here are six key ways I think we can make lung cancer screening possible:
1. Rigorous selection criteria. NLST showed a mortality benefit, but the government purse is tight and some doubts exist about the value of lung cancer screening. A recent study in the New England Journal of Medicine showed that within NLST subgroups, some people are at higher risk for death due to lung cancer than others.
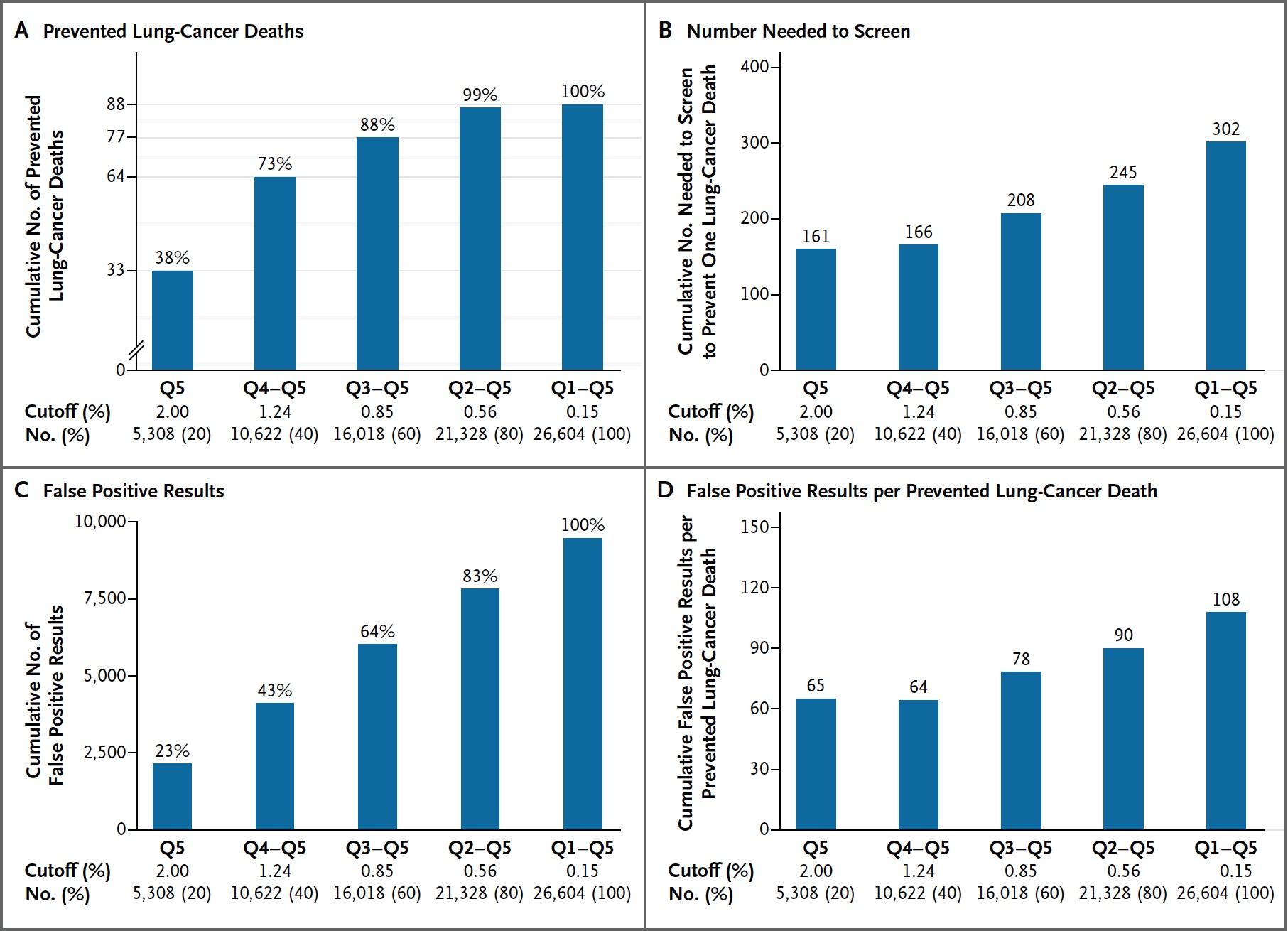 |
Figure 1: Kovalchik et al, NEJM 2013. |
Focusing upon high-risk patients makes sense. Currently both USPSTF and National Comprehensive Cancer Network (NCCN) agree that patients 55-74 with a 30+ pack year history and smoking cessation <15 years should be screened. A recent joint statement from 41 organizations favors screening up to age 80 in people healthy enough for curative treatment. The consensus statement requests coverage with evidence for some selected patients also at higher risk. The decision to screen should be based upon risk, not age.
2. Decreasing false positives. A major concern expressed at MEDCAC was the problem of false positives leading to additional testing/lung biopsy—a legitimate point. The morbidity of biopsy is also higher than that of breast or prostate cancer. Dr. Peter Bach from Memorial Sloan-Kettering Cancer Center suggested that risk may go up with age.
 |
Figure 2: Peter Bach at MEDCAC, YouTube, http://bit.ly/MEDCACam. |
However, he also acknowledges in passing that since NLST’s design, the quality has already improved. Now there are better criteria to help define which lesions to biopsy. This recent analysis strongly suggests that the false-positive rate can be lowered, and the American College of Radiology is finalizing standards based upon the LungRADS model to ensure the risk of false positives is minimized.
3. Addressing “scanxiety”. At the MEDCAC hearing, some skeptics raised concerns about the anxiety of screening with imaging. In my opinion, this is one of the weakest arguments against screening. First, there is no good evidence to suggest that screening results creates enough anxiety to negate the value of screening. Anxiety and depression medication use isn’t higher and quality of life is similar in screened compared to non-screened patients. Mammography still has a net benefit, including from the patients’ perspective. Second, it is an opportunity to encourage smoking cessation. Combining smoking cessation with screening can improve the cost effectiveness of screening and will have additional non-cancer health benefits. Anxiety is natural when someone becomes aware of a health risk; that doesn’t mean we shouldn’t screen.
Third, I think we should also take into consideration the anxiety of newly diagnosed patients. Anxiety increases with more advanced stage; so does depression. Anecdotally, many of my patients with prostate or breast cancer (once diagnosed) express positive feelings about how screening helped catch it earlier. In lung cancer, this sense of being proactive may help with smoking cessation rates and tolerating treatment. We can lessen the degree of scanxiety with education and shared decision-making.
4. Cost control. Lung cancer screening will cost money, no doubt. But the widely reported estimate is currently in an abstract only, which hasn’t even been presented! Published data suggest that low-dose CT screening is cost effective compared to other cancer screening tests. Critics point out correctly that possible work productivity benefits for those age 50-64 may not apply in older patients. But more people continue to work beyond age 65 because they have to, so there still would be possible real economic benefits.
5. Accurate risks of treatment. Dr. Peter Bach spoke eloquently at the MEDCAC meeting, citing higher surgical mortality rates in older patients (Fig. 2). While true, it’s misleading. Increasingly, stereotactic ablative radiation can offer excellent disease control with very low mortality in medically inoperable patients and compares favorably to surgery. The median age in the first study, RTOG 0236, was 72 years old. It’s already standard for many elderly, medically inoperable patients. Maybe Dr. Bach just didn’t know.
6. Quality of the screening program. Participating community sites in NLST were collaborating with academic centers. Whether a community hospital can reproduce these results may depend upon multiple factors. Reimbursement may create a financial market for any hospital to say they can offer lung cancer screening. Dr. Bach pointed out that not all community sites may be able to offer appropriate quality services.
I agree with Dr. Bach on this point. The likelihood of harm from a poorly designed screening program may increase costs by over-treating patients, the right and wrong ones. One way to address this issue would be to develop a screening program certification process and reimburse only certified programs. In fact, the joint statement to Centers for Medicare & Medicaid Services recommended that certain quality standards established by the American College of Radiology are required.
As a cancer specialist seeing a lot of patients die from lung cancer, I see CT screening as a way to avoid that fate for many. As a citizen, I appreciate MEDCAC’s caution in rubber-stamping tests with the potential to be harmful and expensive. But it’s not an all-or-none decision. Hopefully, the Centers for Medicare & Medicaid Services will not restrict access to lung cancer screening based upon age alone.
NOTE:
ASCOconnection.org is a forum for the exchange of views on topical issues in the field of oncology. The views expressed in the blogs, comments, and forums belong to the authors. They do not necessarily reflect the views or positions of the American Society of Clinical Oncology.
Dr. Matthew Katz has no relevant relationships to disclose.
Editor’s Note: This commentary was updated by the author on July 1, 2014.


Recent posts