Each time I reach the point of recommending radiation treatment for someone with a brain tumor or head and neck cancer, I ask for a higher level of trust from each patient than usual: let us make a mask to keep you safe.
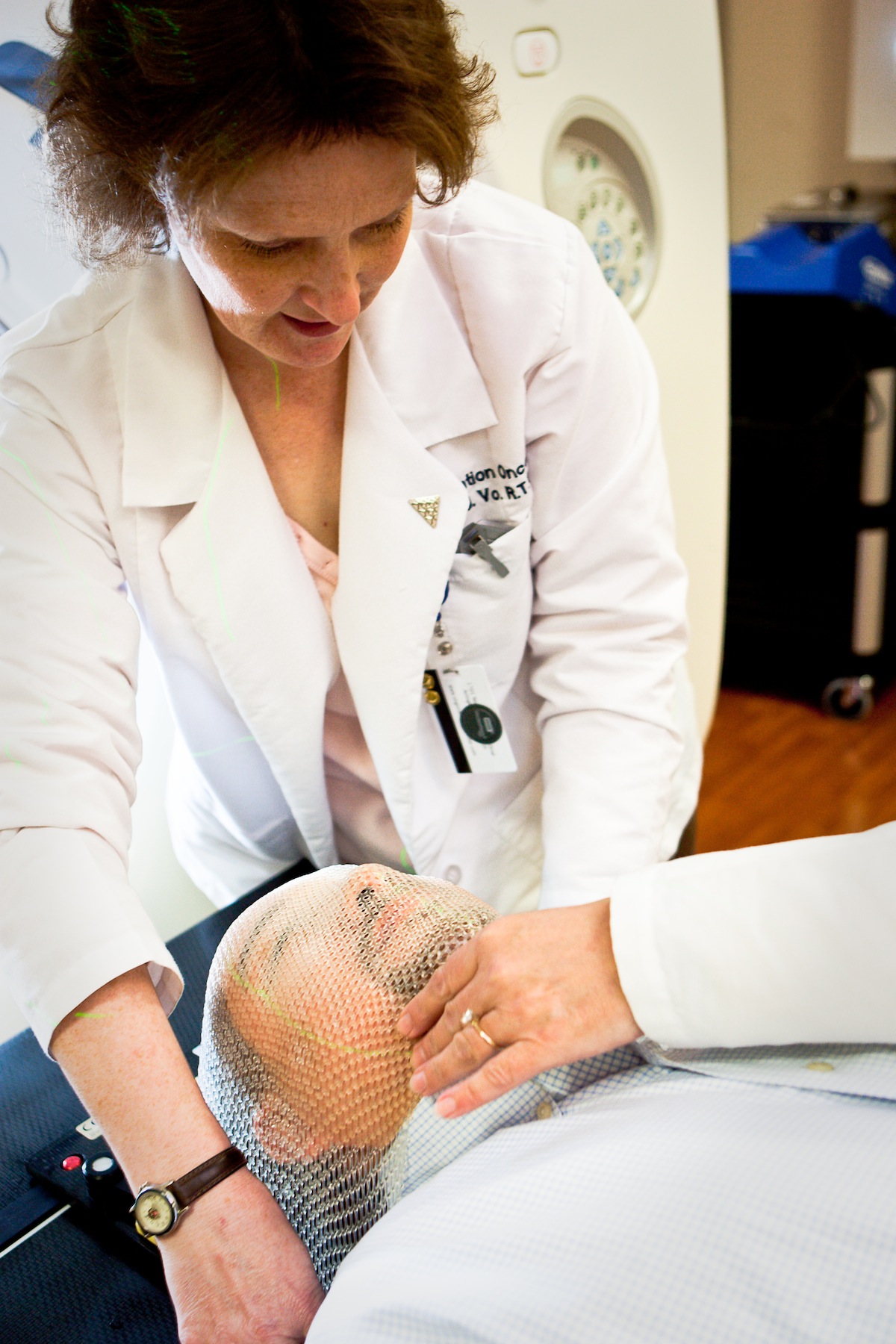 | |
| Photo credit: ASTRO/Adam Donohue or RTAnswers.org/Adam Donohue |
In the U.S., there are 40,000 people each year with a new primary brain tumor, a similar number with head and neck cancer, and over 100,000 with brain metastases. That’s tens of thousands that require a mask each year. Sometimes people need more than one treatment course and have to go through it again. And again.
From a safety standpoint, the mask is essential. Less movement means more precision and accuracy, which can translate to fewer side effects. In some cases, like stereotactic radiation, immobilization permits me to give radiation doses that couldn’t be done effectively any other way. But that doesn’t mean it’s easy on patients or their loved ones who help encourage them each time before getting on the table.
When you lie down for planning, the therapists take warm, wet plastic from a waterbath and lay it over you. Gently smoothed to fit well, the mask hardens as it cools. It’s a mold that provides a durable, reproducible position for treatment. But that mask also becomes an enduring, tangible relic of cancer treatment. A plastic sculpture capturing a snapshot of the cancer experience, and the hopes and fears that go with it.
Some don’t want to see it again. Some want to take it home to destroy, while others may want to hang it on the wall, a badge of courage. Another fascinating approach has been using that mask for self-expression, creatively displaying that courage for others. Sometimes sharing can make it easier, a chance to celebrate life after treatment.
Claustrophobia is fairly common. I can prescribe medication to make it easier, but I suspect some of the anxiety is the fear involved in making such a leap of faith. It’s one thing when I already know the patient, but often that’s not the case.
We can do a better job of preparing patients, making that leap of faith a little less daunting. There are educational materials available, and we can talk about it. But I think better yet would be to see the process, to make it less of an unknown.
So I’m going to video the process, with myself as the patient. The effort on our part may make it easier for patients to have faith in us. So I ask you, patients, advocates and doctors: what do you want to see?


Comments
Mary Joanne Deforest
Aug, 28 2013 9:05 AM
It didn't bother me. A large part of it was the trust I had in my radiologist, Amit Garg, MD in Albuquerque. For me there was just something that clicked. When my mask was made, they were happy and surprized that I could move to adjust my position. So many people get so scared they can't move. I had one problem-part of my nose was surgically removed, and it gave me sinus problems. One time a mucous plug broke loose and lodged in my throat. I started to panic. Then I remembered that I could swim underwater, and I was in the thing for less then 10 seconds. When it was over with, I wanted that mask off. It never dawned on me to raise and wave my hand. I raised my leg-I was wearing jeans-and waved my foot.
Maybe it helped that I'm from uranium country, and my son was an underground miner. I sleep with a radioactive hard hat above my bed. I used to live in a house with a porch made from radiactive timbers-I was diagnosed with aggressive, atypical BCC in the nose lip from the sun. I'm sure that my washing machine was raioactive after a few months of washing his coveralls.
Then I have a basic understanding how radiation works. I was more concerned about blasting caps in his pockets.
My post-rad CAT with contrast showed all of the cancer tumors gone. I'm enjoying today-I should enjoy tomorrow. I'm so thankful that I'm not in Houston with my nose, eye, and the bone-flesh removed from the right side of my face, waiting a prosthetic face. I considered that a fate worse than death. Lets face it--Johnny Depp is the only person that looks glamerous with an eye patch. My astronomy prof turned the geiger counter on, and most people were terrified because it read the clickings from buildings. I have my taste buds, can smell, have my teeth, and a moist mouth. Most of all, I'm not a frankenstein locked away in Texas, listening to these discussions about the future of medical care on the news. Thank you doctor for trying to allay people's fears and sometimes giving cancer victims an option.
Matthew S. Katz, MD
Aug, 28 2013 9:38 PM
Thank you Mary for sharing your experience. It sounds like you had a great treatment team and have done wonderfully. I highlighted in this post some of the anxiety that may come with radiation masks, but you make an important point - most people do very well with them.